(RxWiki News) As the number of Americans with type 2 diabetes continues to grow, more and more patients are suffering from complications like foot infections. Fortunately, proper care can reduce these complications.
Foot infections have become a more common problem among diabetes patients. But new guidelines suggest that the right treatments can prevent amputation and save lives.
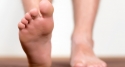
"Take care of your feet if you have diabetes."
When a foot infection goes untreated, people with diabetes are faced with the possibility of a foot or leg amputation. Around 50 percent of diabetic amputees die within five years.
If patients and doctors took proper care of foot infections, about half of amputations could be avoided, according to new guidelines from the Infectious Diseases Society of America (IDSA).
The guidelines were written by Benjamin A. Lipsky, M.D., of the University of Washington, and his colleagues at IDSA.
Foot infections are common among people with diabetes because many patients have poor blood flow and little feeling in their feet. If even a small sore or cut goes unnoticed, it can get infected. Without the proper care, the infection can get worse, spreading to other tissue and bone.
This infected tissue may need to be removed. For some patients, removing tissue may mean removing a whole toe, foot, or even part of a leg.
As many as one out of four diabetes patients will have a foot ulcer (open sore) in their life. About 85 percent of diabetes-related amputations start with a foot ulcer.
"Lower extremity amputation takes a terrible toll on the diabetic patient," says Dr. Lipsky.
"People who have had a foot amputated often can no longer walk, their occupational and social opportunities shrink, and they often become depressed and are at significant risk for a second amputation," he explains.
"Clearly, preventing amputations is vital, and in most cases, possible," he says.
The new guidelines stress the importance of treating foot infections quickly and properly. This may include removing small sections of infected tissue and using antibiotic drugs. In some cases, a doctor may take pressure off the wound and improve circulation to the infected area.
The guidelines also suggest using a team of experts from different fields to treat diabetic foot infections.
Since the last IDSA diabetic foot infection guidelines were released in 2004, new research has shown that many foot infections do not receive the proper care.
The new guidelines provide doctors with 10 questions to ask themselves as they treat diabetes patients with foot wounds.
The first thing a doctor should do is check if the wound is infected. An infected wound, according to the guidelines, is likely to be red, warm, tender, painful, or swollen.
If a foot wound has become infected, doctors should use imaging technology to see if the bone has become infected. Doctors should also take a tissue sample to see what kind of bacteria is causing the infection. Knowing the type of bacteria can help doctors choose the right antibiotic drugs.
According to Warren S. Josepeh, DPM, a consultant at Roxborough Memorial Hospital in Philadelphia and co-author of the guidelines, "There is quite a bit of overprescribing or inappropriate prescribing of antibiotics for diabetic foot wounds, which doesn't help the patient and can lead to antibiotic resistance.
"The guidelines note that when antibiotics are necessary they should be discontinued when the infection is gone, even if the wound hasn't completely healed."
The guidelines appear in the journal Clinical Infectious Diseases.