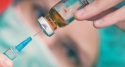
(RxWiki News) There's no guarantee of avoiding any kind of cancer, but some cancers have better chances for prevention than others. Several practices can help prevent cervical cancer, but do all doctors follow them?
A recent study found that only about half of the studied OB/GYNs reported following the cervical cancer screening guidelines issued in 2009 by the American Congress of Obstetricians and Gynecologists (ACOG).
Less than a third of these OB/GYNs reported that their patients had been vaccinated against human papillomavirus (HPV).
HPV is a sexually transmitted infection that can cause cervical cancer. The vaccine series includes three shots and the ACOG recommends it for most females aged 11 to 26.
"Ask your OB/GYN about cervical cancer prevention."
This study, led by Rebecca B. Perkins, MD, of the Boston University School of Medicine, aimed to better understand attitudes and practices related to cervical cancer screening guidelines in the US.
The current ACOG recommendations for preventing cervical cancer include the following:
- Giving the HPV vaccine
- Starting cervical cancer screening for patients at age 21
- Screening every two years for patents aged 21 to 29
- Screening every three years for women aged 30 and older
- Testing for HPV during routine Pap tests for women aged 30 and older
- Discontinuing screening for patients over age 70 or after a hysterectomy for non-cancer-related reasons
The HPV vaccine protects against the four strains of HPV that are responsible for causing the majority of cervical cancer cases.
The researchers reported on the results of a 15-item questionnaire completed by 366 OB/GYNs from 2011 to 2012. The doctors were an average age of 53 and had spent an average 21 years in practice. About half were male and most were white.
The OB/GYNs were all members of the ACOG and answered questions about their demographics, clinical practices and the barriers they perceived related to HPV vaccination and cervical cancer screening.
The study's results showed that only 27 percent of the OB/GYNs estimated that the majority of their eligible patients (at least 60 percent) had started the HPV vaccine series even though 92 percent of them said they offered the shot.
The biggest barrier the OB/GYNs reported was refusal to get the vaccine by patients and/or their parents. About 56 percent of parents declined to have their daughters vaccinated, and 22 to 42 percent of young women themselves declined it.
The doctors also showed some concerns about recommending the vaccine to younger patients. Although 96 percent would recommend the vaccine for a 13-year-old patient, only 73 percent would recommend it to an 11-year-old, and men were half as likely as women to offer the vaccine to children aged 11.
However, "Approximately 80 percent to 90 percent of physicians adhered to guidelines recommending vaccination to women with a history of multiple partners, abnormal Pap, or genital warts, and up through age 26 years," the authors wrote.
Other barriers to immunization included financial barriers, cited by 23 percent of the doctors, and simply forgetting to recommend it to a patient, cited by 21 percent of the doctors.
Only 1 to 2 percent of the doctors expressed any concerns about the vaccine's safety or effectiveness, and 31 percent reported they experienced no major barriers to vaccination.
Women who are breastfeeding can safely receive the vaccine, but only 40 percent of the doctors offered it to such women. Meanwhile, pregnant women are not recommended to receive the vaccine even though 10 percent of the doctors surveyed said they offered it to pregnant women.
The survey results also showed notable differences in how closely OB/GYNs followed the guidelines on cervical cancer screening with Pap smears.
Approximately one half of OB/GYNs started and stopped cervical cancer screening for women based on the guidelines. The recommendations are to begin screening at age 21 and discontinue at age 70 or after a hysterectomy in low-risk patients.
While 57 percent said they began screening patients at age 21, 45 percent said they stopped screening patients at age 70. Men were half as likely as women to stop screening at age 70 or after a hysterectomy.
Although Pap smears are no longer recommended annually, many of the respondents still do them each year: 74 percent of the OB/GYNs said they screened patients aged 21 to 29 annually, and 53 percent screened patients aged 30 and older annually.
The reasons for this finding appeared to be related to perceived patient preferences. "More than 70 percent of physicians felt that patients were uncomfortable screening less frequently than annually, although 81 percent stated that they were personally comfortable with extended intervals," the authors wrote.
About half of the OB/GYNs, however, expressed concern that women would not come for their annual exams if the doctors did not conduct annual Pap smears.
Although the recommendations include co-testing HPV and Pap, only 45 percent offered co-testing to women aged 30 and older. Another 21 percent offered it if the patient requested it, 11 percent screened all women with both tests and 23 percent did not test for HPV at all.
Doctors who worked in solo practices were less likely to follow the recommendations for vaccination and screening than doctors who worked in group practices.
OB/GYNs in group practices were more than five times more likely to offer the vaccine than doctors working solo in their own practices.
Overall, only 4 percent of the respondents (16 doctors) followed all of the 2009 recommendations for cervical cancer screening.
"Unfortunately, survey results indicated that more physicians followed non-evidence-based practices, such as continuing screening for women aged over 70 years and for those who had hysterectomy for benign indications, than adhered to current evidence-based recommendations," the authors wrote.
They suggested that programs to educate doctors and patients on the evidence behind HPV vaccination and non-annual cervical cancer screenings may help improve cervical cancer prevention efforts.
This study was published July 9 in the American Journal of Preventive Medicine.
This research was funded by an American Cancer Society Mentored Research Scholar Grant and by the Department of Health and Human Services, Health Resource and Services Administration, Maternal and Child Health Research Program. The authors reported no conflicts of interest.